Consider manufacturing ARVS locally, Govt urged
Abigail Mawonde Herald Correspondent
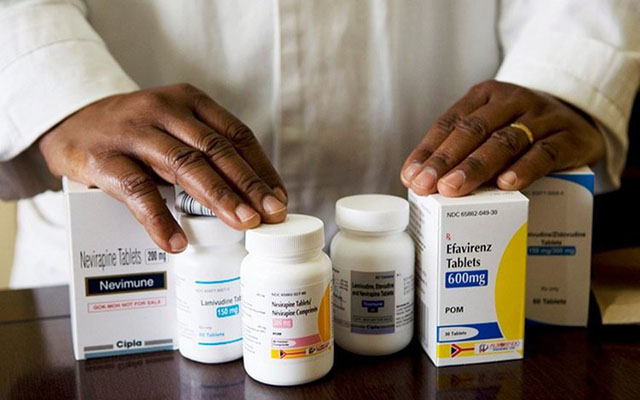
Government has been urged to consider manufacturing Anti-retroviral drugs locally to avert shortages in future. Addressing journalists in Harare on Wednesday, Zimbabwe National Network of People Living with HIV national chairman Mr Sebastin Chinhaire said shortage of the drug was affecting many people living with the virus in the country. “The Zimbabwe National Network of People Living with HIV (ZNNP+), Zimbabwe Lawyers for Human Rights (ZLHR) and the Diocese of Mutare Community Care Programme (DOMCCP) express grave concern over the slow pace at which the ongoing shortages of anti-retroviral drugs (ARVs), particularly the second line regimen drug — Abacavir — is being resolved,” he said.
“These shortages put the health and welfare of over one million people living with HIV at risk.” Mr Chinhaire said Government should ensure the problem was resolved urgently.
“Over the past two months, we have noted with concern that thousands of people living with HIV have been caught up in the ongoing shortages of the life-saving second line ARV drug — Abacavir,” he said. “We are equally concerned that the country will not be able to cope if the clients on second line have to be moved to the third line (a much more expensive combination) due to treatment failure and an increase in defaulters due to unavailability of treatment in public health institutions.”
ZLHR projects lawyer Mrs Agnes Muzondo said manufacturing ARVs locally would help prevent interruptions caused by time lags. “We support calls for the localisation of the manufacture of ARV drugs,” she said. “This will assist in preventing interruptions caused by time lags and potentially bring down the prices of ARV drugs. This is of significant importance considering that this year we celebrate the enrolment of one million people onto the national anti-retroviral therapy programme.” Mrs Muzondo urged Government to make ARVs available to people living with HIV and Aids free of charge to reduce morbidity and mortality.
She said while the three months’ ART supply for clients on the first line treatment regimen was commendable, they were urging the Ministry of Health and Child Care to provide at least six months’ supply for people living with HIV in high emergency alert areas, commonly affected by floods in emergency settings. ZNNP+ national stigma index coordinator Mr Tonderai Chiduku implored Government to put in place requisite mechanisms to curb drug shortages.
“We appeal both to the Ministry of Finance and Economic Development and the Ministry of Health and Child Care to avail the desperately needed foreign currency to ensure an uninterrupted supply of the lifesaving drugs, especially considering that people living with HIV on second line are already at high risk,” he said.









Comments