When craving overtakes sense of judgment
Obert Chifamba Agri-Insight
THE Mekeo tribe of New Guinea believes hunger for plant-foods comes from the abdomen while that for meat starts in the throat. And the Sanumá Indians of Northern Brazil add that no amounts of cassava bread, bananas or any other food stuff can placate that hunger.
It seems the above assertions sum up the situation some people in Zimbabwe find themselves in and end up throwing caution to the wind and devour contaminated meat.
In recent times, cases of people getting hospitalised or dying after consuming beef infected with anthrax have been on the rise, so far 86 people have been hospitalised.
It seems people are listening more to the whims of the belly than to their sense of responsibility.
Such cases have been reported in Bikita, Gokwe, Makonde, Chegutu, Mazowe and Sanyati, to name a few.
These incidents may be just a tip of the iceberg, as many other cases may easily go unreported while others may have been lost with the passage of time.
Most of the cases have been published, which makes it common knowledge that anthrax-infected meat should not be eaten.
The big question, however, is why people are still that reckless to eat cattle dying from the disease when the Department of Veterinary Services (DVS) officers and health experts always preach that animals succumbing to anthrax must not be eaten, as it can also affect people.
Of course, people easily blame their actions on failure to raise the money to buy beef or other meat options, but this does not justify endangering their lives and those of other unsuspecting consumers.
Of late, many people in and around Harare have been on high alert following a spate of cases in which unscrupulous dealers have reportedly been taking cattle affected by theileriosis, also known as January Disease, from rural areas to abattoirs and butcheries in towns.
DVS has always made it clear that people must not eat meat from such animals, but for some strange reason or maybe desperation, people are ignoring the warnings.
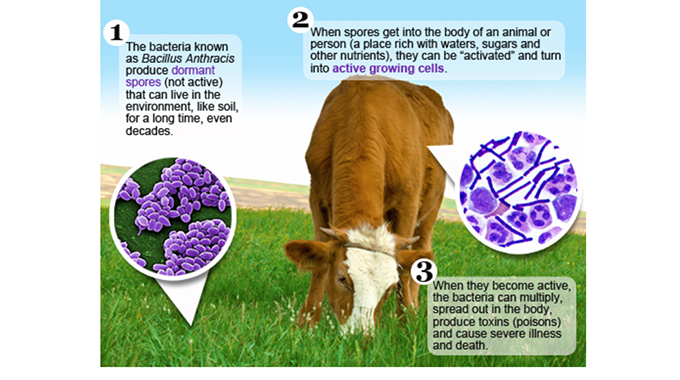
Anthrax is a serious infectious disease caused by the spore-forming bacterium bacillus anthracis. The bacteria can be found naturally in soil and is resistant to drying and disinfection, and can remain alive in contaminated soil for decades.
Anthrax commonly affects domestic and wild animals.
It is primarily a disease of plant-eating (herbivorous) animals such as cattle, sheep, goats, camels and horses. Disturbed grave sites of infected animals have been known to cause infection after 70 years.
People generally get sick with anthrax if they come in contact with infected animals or contaminated animal products.
The disease is primarily an occupational hazard of veterinarians, agriculture and wildlife workers, or workers who slaughter animals or process meat, hides, hair and wool.
In fact, anthrax was historically called “woolsorter’s disease” because it was so common among workers in the wool, hides and tanning industries.
Signs and Symptoms
The type of illness a person develops depends on how anthrax enters the body.
All types of anthrax can eventually spread throughout the body and cause death if they are not treated with antibiotics.
Infection can occur in four forms:
Cutaneous: Caused by the bacterium entering a cut or scrape on the skin.
This is the most common form of infection with anthrax, accounting for more than 95 percent of naturally occurring human cases. Infection usually develops within one to seven days after exposure with sores most commonly found on either the face, neck, arms or hands.
Cutaneous anthrax begins as a raised itchy bump that looks like an insect bite, but within one to two days becomes a painless sore, usually one to three centimetres in diameter, with a typical black area in the centre.
Lymph glands near the infected area may swell. Deaths from cutaneous anthrax are rare because the illness can be cured with appropriate antibiotics. Without treatment, up to 20 percent of cutaneous anthrax cases may result in death.
Inhalation: Caused by breathing in anthrax bacteria or spores. The spores are too small to be seen by the naked eye and have no special colour, smell or taste.
This is considered the deadliest form of anthrax and the form most often associated with bio-terrorism.
Infection usually develops within a week after exposure, but it can take up to two months.
Inhalation anthrax begins with mild cold or flu-like symptoms, which include: fever, chills, malaise, mild cough or chest pain.
Symptoms progress to respiratory distress with stridor (vibrating noise when breathing), hypoxemia and cyanosis (bluish colouring of the skin due to low oxygen).
Death from inhalation anthrax can be greater than eight percent if left untreated. However, early diagnosis and aggressive treatment can increase survival rates.
Gastrointestinal: Caused by eating raw or undercooked meat from an animal infected with anthrax.
Gastrointestinal anthrax is the rarest form, difficult to recognise.
Infection usually develops from one to seven days after exposure. Gastrointestinal anthrax is characterised by an acute inflammation of the intestinal tract.
Initial signs of nausea, loss of appetite, vomiting, and fever are followed by abdominal pain, vomiting of blood, and severe diarrhoea. Lesions have been found in the intestines and in the mouth and throat. Without treatment, more than half of patients with gastrointestinal anthrax die. However, with proper treatment, 60 percent of patients survive.
Transmission
Domestic and wild animals such as cattle, sheep, goats, antelope, and deer can carry the disease. Humans can become infected with anthrax by handling products from infected animals, by breathing in anthrax spores from contaminated animal products or by eating raw or undercooked meat from infected animals. Anthrax cannot be spread from person to person.
Humans can also be infected deliberately by terrorists using anthrax as a weapon.
Doctors have several options for treating patients with anthrax, including antibiotics and antitoxin. Patients with serious cases of anthrax will need to be hospitalised. They may require aggressive treatment, such as continuous fluid drainage and help breathing through mechanical ventilation.
For symptomatic gastrointestinal anthrax and inhalation anthrax, large doses of intravenous (IV) antibiotics are needed immediately. Early antibiotic treatment of anthrax is essential — any delay lessens chances for survival.









Comments