Village health workers first line of defence in fight against measles
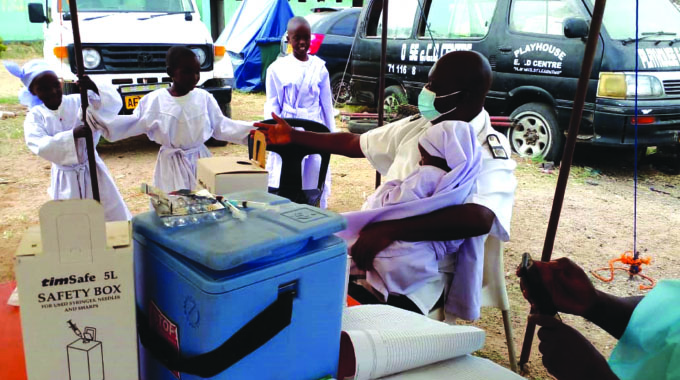
Muchaneta Chimuka
Herald Correspondent
“Equity is a key concern. Covid-19 has the greatest impact on communities that are already vulnerable and marginalised, especially those with high levels of diseases and which have less access to essential health services. The principles of Universal Health Coverage (UHC) still hold in a pandemic; we must meet the health needs of the most vulnerable at all times.”
The above words from Dr Alex Gasasira, the World Health Organisation (WHO) representative in Zimbabwe, tally with the efforts that are being made by Village Health Workers (VHW) in fighting the re-emergency of child killer diseases to meet the full scale of herd immunity.
These village health workers’ primary role is to advocate for underserved individuals or communities to receive services and resources to address health needs.
Village health workers collect data and relay the information to stakeholders to inform programmes and policies. They also provide informal counselling, health screenings, and referrals and build community capacity to address health issues.
VHWs are essential as they help to relieve the substantial burden of the disease outbreaks and pandemics on healthcare systems worldwide.
A recent visit to Mahusekwa District Hospital and Chihota Rural District Hospital in Mashonaland East revealed that these workers have a bigger role in complimenting the Ministry of Health and Child Care’s efforts in as far as health delivery systems are concerned.
Marondera District Medical Officer Dr Delight Madoro said there were positive achievements brought through the support from VHWs. “We are quite happy with the number of children that are being vaccinated against measles, parents are now forthcoming, and they are no longer hiding their children in homes because the majority now understand the negative consequences of shunning immunisations. They have seen death in their communities.
“We applaud VHWs for educating them on the importance of immunisation. They conduct door to door visits encouraging communities to adopt good health seeking behaviour.
“More so, they reach the hard to reach areas using their bicycles. They were trained on good communications skills which enable them to gain acceptance from some members of the apostolic sects who were not willing to take up the vaccination drive, which saw 86 percent of the children in Mashonaland East getting immunised during the Immunisation Expanded Programme (IEP),” he said.
Dr Madoro said during the early days of the first vaccination campaign on measles and rubella, they managed to vaccinate 25 984 children against a target of 30 376, which translates to a percentage of 86 percent and it has not been a smooth journey to achieve this due to some communities that are vaccine hesitant.
“We managed to take samples from the 80 suspected cases and we have so far received 27 results as we await for the remaining difference,” he said. “Out of the 27 results, six of them were measles positive, hence we comment the remarkable efforts by VHWs.”
Dr Madoro said 80 suspected cases of measles were notified by VHWs and they managed to quarantine the suspected to minimise the spread of the disease.
“With trainings on prevention and appropriate infection-control measures, VHWs also serve as good examples of how to prevent measles and polio in the communities they serve,” he said.
“In Marondera District we have a robust immunisation programme where we see children being vaccinated at all our health facilities.
“However, we have heard of about 12 unreported cases of children who are suspected to have succumbed to measles mainly due to some religious groups who are still shying away from seeking medical care in health facilities.
“Therefore, it is the duty of the media and CWHs to educate communities on the importance of immunisations that they save lives and will not affect their religious and traditional beliefs in whatever way. Those cases were not confirmed; hence they remain as speculations,” he said.
Dr Madoro said measles could be prevented and treated if people visit health facilities on time. “Measles is a severe disease caused by a virus and it is normally passed through direct contact with an infected person and through infected air. Anyone who has not had measles before and has not been vaccinated can get it. Unvaccinated children under the age of five are at more risk of measles and its complications, including death. Unvaccinated pregnant women are also at risk,” he said.
Marondera district nursing officer Mrs Marian Fadzi said people were still coming for vaccination and most of them were from apostolic sects. Chihota Rural District Hospital acting sister-in-charge Ms Evelyn Zvomuya said they were targeting influential people in apostolic sects for their awareness campaigns.
“We have taken the participative approach in disseminating information, through the identification of one or two members of an apostolic church who will then go and encourage others to get their children vaccinated,” she said.
“Through the intervention of CHWs, we have surpassed our target of 85 percent vaccination and we are now at 124 percent.”
Community health worker, Mrs Easter Bonda said they were working with local leaders in mobilising people to have their children immunised. “We work as community advocates, conducting outreach and community engagement for public health programmes and provide health education and services,” she said.
“During this measles outbreak, we have been champions for the immunisation drive though working closely with chiefs, village heads and the nursing staff in our area.
“We even accompany some members of the community to the nearest health facilities, hence we have ‘baptised and converted many’.”
Chihota community health worker, Ms Beaullah Chipeni (62), said they had been trained by the Ministry of Health and Child Care and other partners to generate and use data to make informed decisions and improve access to essential health services.
“During our community information dissemination programmes, we educate people on how measles spreads through coughing and sneezing or direct contact, hence we encourage quarantining of sick persons and the importance of seeking emergency care at health facilities such that we do not end up having the whole community infected,” she said.
“The signs of measles include a hot body, rash which starts on the forehead, neck and then covers the whole body and running nose and eyes, red eyes, diarrhoea and white spots in the mouth. If not treated early, the child may develop a severe cough, pneumonia, blindness, deafness and malnutrition and it can lead to death.”
Mrs Naomi Mangwanya, who had visited Mahusekwa Hospital to have her twin children vaccinated against measles and polio, said she was motivated by the village health workers.
“CVHWs in our communities are the ones who told us that the vaccination programme is still on at the hospital and local clinics,” she said. “Some were assuming that the programme is over, therefore, we thank them for bringing the messages right at our door step.
“Due to the escalation of social media use, people do send wrong information, but VWHs are trusted because we know they work closely with nurses and they stay in our communities. We have seen death in our communities and that is also pushing so many parents to adhere to the children’s primary immunisation course that should be completed before their first birthday,” she said.
Executive director for Community Working Group on Health, Mr Itai Rusike said the principles of Universal Health Coverage relied on equitable and resilient health systems.
“The empowerment of VHWs is crucial in maintaining availability and access to essential health services. When people have the right information at the right time it makes all the difference in saving lives, providing treatment and preventing diseases,” he said.
“Monitoring and analysis of health systems, followed by practical support, is vital to the decision-making process across the health system. It cultivates good health seeking behaviour and it saves lives. A good example is what was happening in Manicaland Province where some members of the apostolic sect were hesitant to immunise their children. Several tactics were employed, including the use of VHWs and we are now witnessing positivity in case reduction and deaths,” he said.
Apostolic sect members, who have previously objected to vaccination, are now warming up to the ongoing measles vaccination blitz after the disease has killed over 500 people and affected over 2 000 others.
The measles outbreak was first recorded in Manicaland province on April 10, 2022 and has since spread across the country and it’s is being contained due various interventions by Government.
Government embarked on a nationwide blitz of polio immunisation targeting the under-fives from October 27 to 30 in the first phase of the campaign, with the second phase starting from December 1 to 4 December.
Zimbabwe had managed to eliminate polio, with the last case having been detected in 1989, while the World Health Organisation certified the country free of polio in 2005.
World Health Organisation (WHO) Zimbabwe, with support from the Universal Health Coverage Partnership, has worked closely with the Ministry of Health and Child Care, and provided technical assistance to strengthen the delivery of essential health services at rural, district and provincial health facilities — both prior to and during the Covid-19 pandemic and disease outbreaks such as measles, cholera, poliomyelitis among others.









Comments