Garment that averts maternal deaths
Roselyne Sachiti Features, Health & Society Editor
In July 2013, Government officials, development partners and women whose lives had been saved by an innovation known as the non-pneumatic anti-shock garment (NASG) gathered at a Harare hotel to share experiences.
The garment was fairly new to Zimbabwe’s public health system and was under randomised trials at Parirenyatwa Group of Hospitals and Harare Central Hospital leaving most stakeholders with the appetite to learn more about it.
One of the women, Tatenda Mugariri, explained how the NASG saved her life the previous year.
Mugariri experienced pregnancy complications at six months, miscarried and bled profusely almost losing her life.
“I was in pain and lost a lot of blood. I started feeling dizzy, my brain started shutting down. The doctor who attended to me suggested that I use the NASG which was on trial at Harare Hospital. The NASG saved my life,” she said back then.
Six years down the line, the Government has rolled out the NASG to other public health facilities mostly in the country’s rural areas with the hope of saving more lives.
Many pregnant women in rural areas because of various reasons — one of them religious beliefs — do not access mothers waiting shelters, another intervention by Government and its partners like Unicef and UNPFA to reduce maternal deaths. Such women face long delays while a decision is made at home to seek care, organise transport, travel to the hospital and wait in the hospital for blood or surgery.
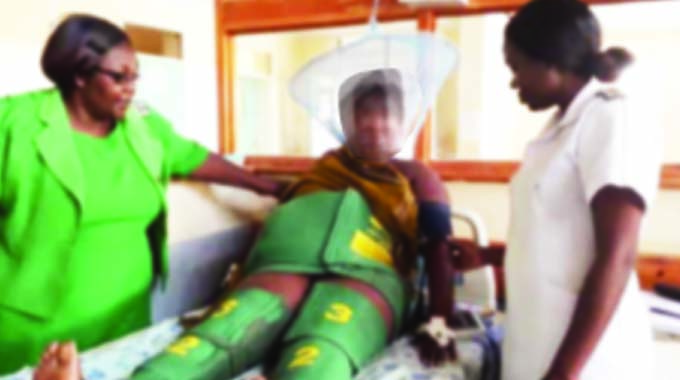
In the absence of the NASG, such women could bleed heavily and die. NASG is a low-technology, low-cost first aid device used to treat shock, resuscitate, stabilise and prevent severe bleeding.
It applies circumferential counter pressure to the lower body and uterus which increases circulating blood to the heart, lungs and brain and decreases the rate of blood flow in the abdomen and pelvis, thus decreasing blood loss. Each garment can be used up to 40 times and is not expensive, an added advantage for under resourced countries like Zimbabwe.
Maintenance is easy as it only requires washing and bleaching. Since its roll out in Zimbabwe, success stories have been told and more women have “escaped the jaws of death” and lived to tell their stories.
The NASG has produced positive results in Zimbabwe proving that the great majority of maternal deaths are preventable with proper antenatal care, skilled delivery at birth, post-partum care and access to emergency obstetric care if complications arise.
It is also testimony of how new technologies, treatments, and other science-backed practices help to decrease maternal deaths and increase life expectancy.
Family Health director in the Ministry of Health and Child Care, Dr Bernard Madzima said the NASG intervention was important in reducing maternal mortality in Zimbabwe.
He said according to the Zimbabwean 2015 Demographic Health Survey, the maternal mortality rate was 651 per 100 000 live births, a figure driven by three main issues: sepsis, eclampsia and haemorrhage (ZDHS, 2015/6).
“Post-partum haemorrhage (PPH) is the major direct cause of these, accounting for 26 percent of maternal deaths among women of all ages (MOHCC First Half Annual report, 2018).
“In recognition of this, the Zimbabwean Ministry of Health and Child Care (MOHCC), with the support of the Clinton Health Access Initiative (CHAI) conducted a three-month rapid process evaluation of the implementation of the non-pneumatic anti-shock garment (NASG),” he said.
Dr Madzima explained how the NASG buys the much needed time to save lives of haemorrhaging women.
“The NASG is a device that can halt hypovolemic shock secondary to blood loss in obstetric haemorrhage. This compression wrap is lightweight, reusable, and fairly simple to apply, making it a suitable tool for low-resource settings.
“While the NASG alone is not a treatment for PPH, it buys essential time to transport haemorrhaging women to a facility, or to a ward within a facility, that can provide the needed services, in order to assure that adequate time is available to deliver life-saving obstetric emergency care,” added Dr Madzima.
He said while the NASG has been proven effective in a variety of studies, including a randomised controlled trial (RCT) conducted in Zimbabwe and Zambia, there remained limited understanding of its operationalisation in rural, low-resourced settings.
“The aim of the process evaluation, therefore, was to understand how contextual factors of the process of integrating the NASG into the obstetric emergency response within the public health system in Zimbabwe contributes to its reach, effectiveness, adoption, implementation and maintenance,” he added.
He revealed that in consultation with MOHCC and provincial management, Hurungwe District in Mashonaland West Province was identified as a high-priority area and selected as the target geography for this process evaluation.
The scope of facilities included 31 rural health facilities, one mission hospital, one district hospital and the provincial hospital. A total of 113 NASGs were distributed to the participating facilities.
“Over the three-month implementation period we carried out activities that include a baseline assessment to ascertain the system readiness for the NASG; procurement and distribution of the NASG and supporting items (such as BP machines and cleaning equipment); training of health practitioners who offer maternal health services and laundry staff; and monthly supportive supervision visits led by the MOHCC district team to ensure the NASG was being utilised correctly and to reinforce best practices.
“Over this period the NASG was successfully utilised on eight patients, out of 11 recorded PPH cases. All women were successfully stabilised and referred for care and treatment, recovered, and discharged home,” explained Dr Madzima.
He said the NASG was well-received by the health care workers, particularly given severe shortages of functional, fuelled ambulances in the district during the implementation period, as the NASG serves to effectively stabilise the woman whilst she awaits transport for referral.
Such steps by Government prove that Zimbabwe is committed to reducing maternal mortality.
Twenty-five years ago, at the International Conference on Population and Development (ICPD) in Cairo, 179 governments, Zimbabwe included, adopted a visionary Programme of Action that aimed to safeguard the health and rights of women and girls and to promote their empowerment.
In 1994, the Programme of Action called for countries to effect “a reduction in maternal mortality by a half of the 1990 levels by the year 2000 and a further half by 2015.” Taken together, this would be a 75 per cent reduction in maternal mortality.
With low cost interventions such as the NASG, health providers can buy time and put the lives of many women out of danger. The country can also move toward reaching its global commitment goals.
[email protected]; [email protected]; Twitter @RoselyneSachiti









Comments