Red flag for maternal health care services
Rumbidzayi Zinyuke Senior Health Reporter
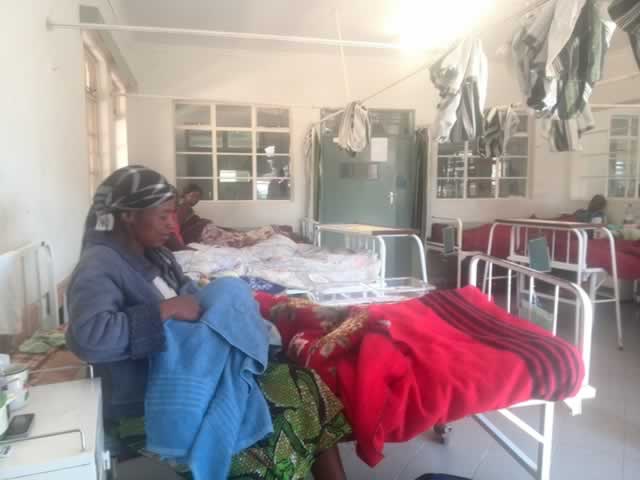
The failure by Harare City Council to offer maternal health services to women in some of its polyclinics could result in an increase in the maternal mortality rates as expectant mothers have to travel longer distances with health experts calling for urgent interventions to protect the lives of women and newborn babies.
The local authority last week admitted that it was struggling to offer services to expecting mothers at Glen View and Budiriro polyclinics due to a crippling shortage of nurses, with only half of maternity nursing posts filled, and with Covid-19 even fewer nurses reporting for duty. The council also recently resolved to close nine clinics in the city citing health personnel shortages.
Matabeleland North legislator Dr Ruth Labode said reduced access to maternal health services was a recipe for disaster as it would have an impact on mortality rates. “This will mean that a lot of women will die and our maternal mortality rate will increase. “.
Zimbabwe continues to record high maternal mortality rates at 462 deaths per 100 000 live births as of 2019. The number may have risen as a result of the COVID-19 pandemic.
Dr Labode said the root cause of the challenge was the skills flight seen in the country as most health personnel seek employment in other countries within the region and beyond.
“It is unfortunate that we have a high number of nurses leaving the country to seek employment elsewhere. Our major challenge is that as a country, our health professionals are not being paid salaries that match what is being offered in other countries so they will definitely go if they get the opportunity. We should look into adjusting salaries of health workers so that they can stay. Currently, we are training for the rest of the region and the world while we are getting nothing for ourselves,” she said.
Last year, more than 2000 health care professionals left the service for other countries, more than double the number that left in 2020.
Community Working Group on Health executive director Mr Itai Rusike said the closure of some council clinics due to human resources challenges needed urgent attention from the responsible authorities.
“It has reduced access to skilled midwives and adds a cost burden and barrier to service uptake for women, indicating the urgent need for the city council to improve the conditions of service for its employees. Apart from the general inputs that all people need for health, women also need services to support reproductive health, pregnancy, prevention of mother to child transmission of infections such as HIV, child delivery and care, including nutrition during pregnancy,” he said.
“Many highly skilled medical personnel have left the public health sector, either for jobs abroad, or in order to enter private practice. Although training has increased in recent years, this is not enough to stop the flow; wages, salaries and conditions of work also need urgent attention.”
To try and proffer solutions to the staff attrition menace, the Health Service Board last year conducted a study to determine the remuneration of health workers in the countries where health personnel are migrating to guide the Government in the restructuring of salaries.
Although the Government increased pay by up to 140 percent in 2021, inflationary pressures eroded the incomes.
“We are not saying the Government should pay our staff the same level as UK or Canada but we want them to see how other countries value and pay their health workers while they compare the conditions of service for local workers with those in Botswana, Namibia, South Africa, Lesotho and other countries whose economies are almost the same as ours and then make a decision,” HSB chairman Dr Paulinus Sikhosana said last month.







Comments